
Augmented reality in healthcare: top 6 use cases, benefits and real-life examples
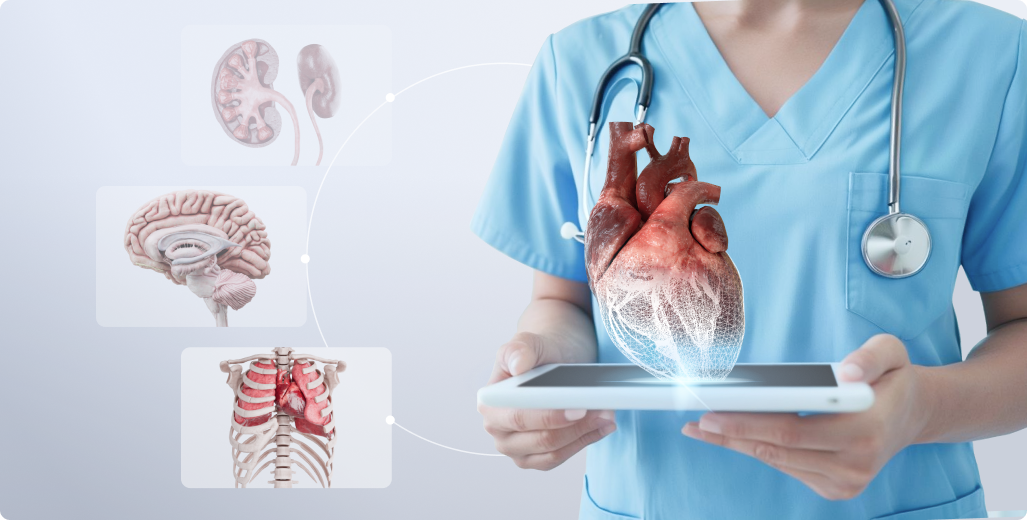
Table of contents
Augmented reality (AR) changes the way medical professionals train, conduct procedures, and engage patients. From supporting complex surgeries to enhancing patient understanding, AR helps improve precision, safety, and engagement across healthcare settings.
This guide explores the top use cases and benefits of augmented reality in healthcare, highlighting how tools like the 3D anatomy atlas VOKA 3D Anatomy & Pathology are making a significant impact in the medical field.
Meaning of augmented reality and its role in healthcare
Augmented reality is a technology that overlays digital information, such as images, data, and 3D models, onto the physical environment. Unlike virtual reality (VR), which immerses users in an entirely digital space, AR enriches real-world scenarios with valuable, context-specific insights.
AR technology is transforming how healthcare professionals (HCPs) work with medical information. Traditionally, they have relied on two-dimensional formats such as X-rays, MRI scans, or textbook diagrams. While these are essential, translating 2D visuals into a 3D anatomical understanding requires significant expertise to cross-reference and interpret data.
AR addresses this challenge by projecting interactive 3D models directly into the user’s view. This makes it easier to visualize anatomy, understand spatial relationships, and interpret complex cases with greater accuracy and speed.
For example, a physician might use AR to demonstrate coronary artery atherosclerosis to a patient on 3D pathology models, highlighting areas where plaque buildup is narrowing the blood vessels. Similarly, an educator showcases a model of lungs affected by tuberculosis in a lecture, so students can interactively visualize how the disease progresses.
In other words, AR in healthcare bridges the gap between digital assets and real-world applications. offering advanced insights and practical applications for both healthcare professionals and patients.
Top 6 augmented reality use cases in healthcare
From making surgeries more precise to helping patients better understand their conditions, AR is proving to be a game-changer. In this section, we delve into the top six ways of how augmented reality is used in healthcare.
1. Surgical planning and assistance
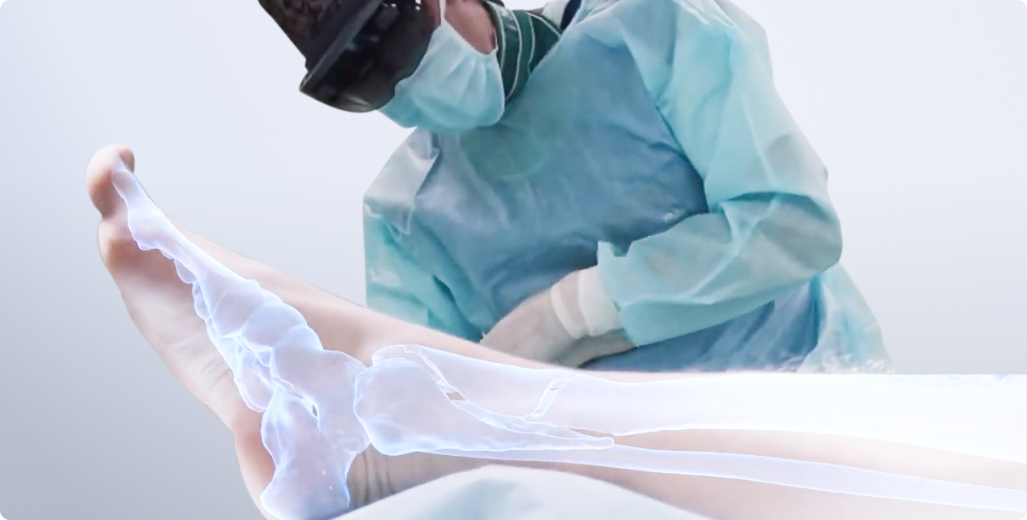
Augmented reality enhances surgical planning and execution, helping healthcare professionals stay focused and informed. AR can become an invaluable tool for preparation and surgical training. Before entering the operating room, surgeons can use 3D models, such as those provided by VOKA, to refresh their knowledge of anatomy. Such detailed, interactive models allow HCPs to explore the body systems from every angle, helping them identify key structures and assess potential risks. With AR, they can virtually map out the procedure and refine their approach.
During surgery, AR continues to assist by offering real-time, precise guidance. Surgeons can wear AR goggles that project 3D images and labels directly onto their field of view, overlaying critical patient data such as CT and MRI scans. These goggles enable them to see hidden structures, such as blood vessels, nerves, and bones, providing a clear and detailed view of areas that might otherwise be difficult to visualize.
This augmented view enhances precision, speeds up decision-making, and reduces the risk of errors, ensuring that surgeries are as accurate as possible.
2. Medical training and education

Augmented reality healthcare applications change the game in training and education. Using AR devices, students can see interactive 3D medical models overlaid onto their physical environment, letting students view and manipulate organs, tissues, and skeletal structures. This helps them understand how all the body systems are connected.
Also, AR can guide students through virtual overlays on real anatomical models or even live peers, helping them visualize structures beneath the surface without making a single incision. This improves spatial reasoning, deepens comprehension, and allows educators to tailor lessons to each learner’s pace and needs.
VOKA 3D Anatomy & Pathology offers hyper-realistic 3D models of normal anatomy and gross pathology, viewable in AR, providing students and professionals with an unprecedented, detailed look at human anatomy.
3. Patient education and engagement

Speaking of patient education and engagement, AR helps to replace static pamphlets and basic verbal explanations with rich, interactive learning experiences. With augmented reality, doctors can display interactive 3D models to explain a patient’s anatomy, illustrate how a condition affects the body, and walk them through possible treatment options. This immersive experience helps patients grasp medical procedures better and reduces anxiety.
This approach encourages patients to take an active role in their healthcare, improving adherence to treatment plans and ultimately leading to better health outcomes. For healthcare providers, AR simplifies the explanation of complex concepts and strengthens the patient-provider relationship.
When patients gain real insights into their condition and a clear understanding of the proposed treatment, they are more likely to follow the plan effectively. Interactive explanations with AR also help them make informed decisions and provide consent for procedures.
4. Rehabilitation and physical therapy

Augmented reality is changing the game in rehabilitation and physical therapy. It's moving beyond traditional exercises and manual feedback to offer dynamic, interactive recovery programs that get results. AR uses motion tracking and virtual environments to create engaging therapeutic experiences. Patients can perform exercises in a gamified setting and see their progress in real time. This immersive approach boosts motivation and ensures patients stick to their therapy programmes.
Also, AR allows for the creation of personalized exercise programmes that are tailored to individual needs and recovery goals. This customized approach guarantees optimal recovery outcomes and minimizes the risk of re-injury. Integrating AR into physical therapy provides real-time feedback on movement quality and performance, increasing patient engagement and promoting proper exercise technique.
Studies prove that AR-based rehabilitation accelerates recovery and improves functional outcomes in various patient populations. This technology also offers significant benefits for therapists, enabling them to monitor patient progress remotely and adjust treatment plans as needed. The future is bright for AR in rehabilitation. It will become even more personalized, adapting to each patient's progress and providing targeted therapeutic interventions.
5. Remote сonsultations and virtual collaboration
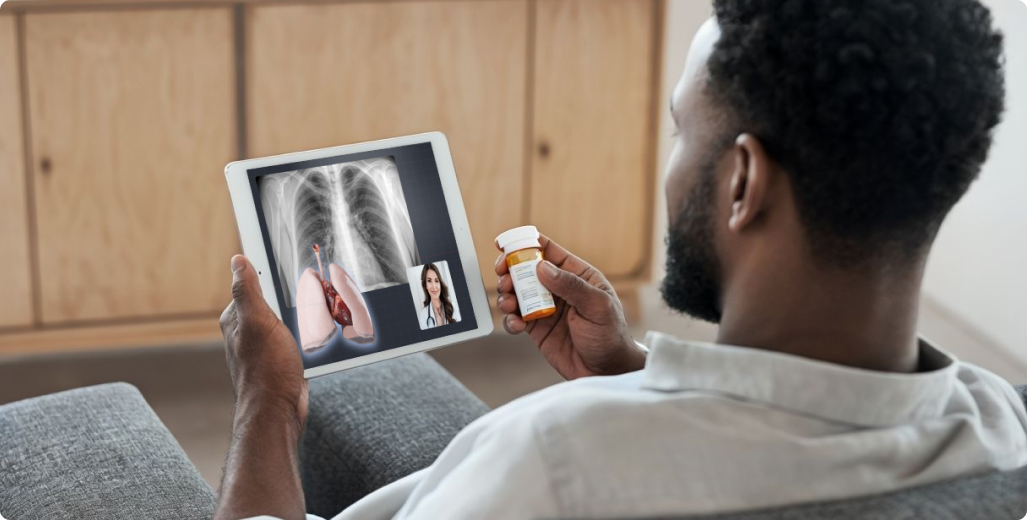
Augmented reality is redefining remote consultations and collaboration by making complex medical information easier for patients to understand. It can significantly enhance how doctors explain conditions and treatment plans during telemedicine sessions.
Instead of relying solely on verbal descriptions or static images, healthcare professionals can use AR to share interactive 3D anatomical models or condition-specific visualizations in real time. For example, during a remote consultation, a doctor might display a detailed 3D model of a patient’s joint to illustrate where cartilage is worn down or use a virtual heart model to show how a valve repair will work. Patients can view these models on their own devices, rotate them, and zoom in to better grasp the details.
AR allows doctors and patients to interact with VOKA's 3D anatomical models during remote consultations. This shared visual platform facilitates more transparent communication and collaborative decision-making.
6. Facility management and surgical room preparation
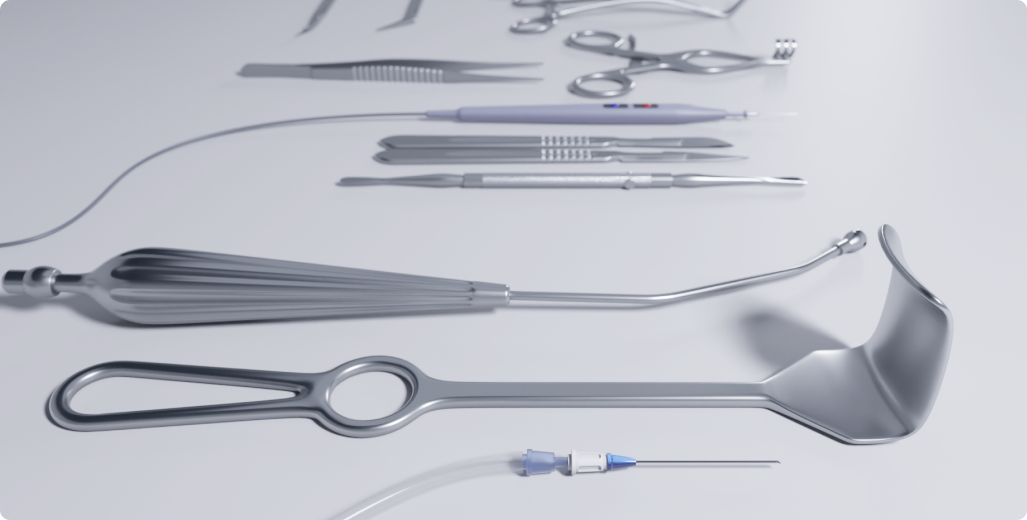
Augmented reality can be a valuable tool for planning and optimizing hospital spaces, including surgical rooms. Instead of relying solely on static blueprints, staff can use AR to overlay 3D models of equipment, furniture, and medical devices into the actual room through AR headsets or tablets. This allows teams to visualize different layouts, test the placement of surgical tools, and rehearse room setups before making physical changes.
Such visual planning helps streamline workflows, reduce unnecessary movement during procedures, and ensure that critical equipment is positioned for maximum efficiency. In surgical room preparation, AR can also be used for training purposes, allowing new staff to familiarize themselves with a room’s layout and equipment arrangement in an interactive, hands-on way without disrupting ongoing operations.
Benefits of augmented reality in healthcare
From enhancing patient outcomes to advancing medical education, here are some of the key advantages that artificial intelligence carries for healthcare:
-
Enhanced surgical precision. AR provides surgeons with real-time, interactive visualizations, offering detailed anatomical views that improve the accuracy of surgical procedures. By overlaying 3D models and labels on the patient’s body, AR helps reduce errors, ensure better outcomes, and speed up recovery times.
-
Transformative medical education. AR allows medical students and professionals to interact with 3D models of the human body, creating a more engaging and immersive learning experience. This hands-on approach enhances retention, facilitates skills development, and provides trainees with the opportunity to practice procedures in a risk-free environment.
-
Reduced anxiety and increased trust. By using AR to explain complex medical procedures and conditions visually, healthcare providers can reduce patient anxiety. Patients gain confidence in their care, feel more informed, and are more likely to provide informed consent, fostering trust in the healthcare system.
-
Better collaboration. AR enables real-time collaboration between healthcare professionals, regardless of location. Specialists can assist in procedures remotely by accessing 3D visualizations, allowing for expert input without geographical limitations. This increases access to specialized care, particularly in remote or underserved areas.
In short, AR is enhancing healthcare by improving accuracy, accessibility, and patient satisfaction, making medical processes more efficient and transparent for both professionals and patients.
Challenges and limitations of AR in healthcare
While the potential of AR in healthcare is vast, several challenges hinder its widespread adoption. One primary limitation is the high cost of AR technology, which can be prohibitive for smaller healthcare providers. This includes the expense of AR hardware, software development, and maintenance, as well as the infrastructure required to support seamless augmented reality applications.
Data privacy and security are also significant concerns, especially as AR systems rely on sensitive patient information. Implementing robust data protection measures is essential, but can be complex and costly. Additionally, AR in healthcare requires extensive training to ensure that practitioners can use the technology accurately and effectively; any misinterpretation or delay in AR visualizations could negatively impact patient safety.
Finally, there are ongoing regulatory challenges, as AR applications must meet stringent compliance standards to ensure safety and efficacy in clinical settings.
The future of AR in healthcare
The future of AR in healthcare looks promising as technology becomes more accessible, affordable, and advanced. As AR hardware evolves, expect to see more compact, powerful devices that are easier to integrate into everyday medical practice. Software advancements will allow for greater accuracy and real-time adjustments, making AR more reliable during complex surgeries and medical procedures.
In medical training, apps like VOKA 3D Anatomy & Pathology showcase how augmented reality in healthcare can provide detailed, interactive models that significantly boost understanding and skill acquisition. While challenges in cost, data security, and regulatory compliance remain, the future of AR is bright.
With further research and development, AR in healthcare could evolve from an innovative option to a standard tool across medical practices, fundamentally changing how healthcare professionals diagnose, treat, and educate.
Conclusion
Augmented reality in healthcare is reshaping the industry by bridging the gap between digital data and real-world environments. With augmented reality healthcare applications spanning surgical planning, training, patient education, and even mental health support, AR is proving to be a transformative force in the field.
In medical training, apps like VOKA 3D Anatomy & Pathology showcase how augmented reality in healthcare can provide detailed, interactive models that significantly boost understanding and skill acquisition. While challenges in cost, data security, and regulatory compliance remain, the future of AR is bright.
As the technology continues to advance, it promises a more personalized, efficient, and informed approach to patient care. With the potential to set new standards of excellence, augmented reality and healthcare are on track to transform how we diagnose, treat, and educate in the medical field.
FAQ
1. What is augmented reality in healthcare?
Augmented reality in healthcare refers to the use of AR technology to overlay digital content, such as 3D anatomical models or instructions, onto the physical environment. This enhances how medical professionals visualize anatomy, perform procedures, and train for clinical scenarios.
2. What are the disadvantages of augmented reality in healthcare?
While the benefits of augmented reality for healthcare are significant, there are some drawbacks. These include high implementation costs, the need for specialized hardware, and a learning curve for both staff and patients. In clinical settings, AR must also meet strict regulatory and safety standards, which can slow down adoption.
3. Is AI used in AR?
Yes, artificial intelligence is increasingly used in augmented reality medical applications, especially in healthcare. AI can improve object recognition, personalize training scenarios, and enhance AR responsiveness. In AR healthcare applications, AI helps analyze data in real time, guide medical procedures, and support informed decision-making.
4. What are the top AR healthcare apps in 2025?
One of the augmented reality application examples is VOKA 3D Anatomy & Pathology, which combines 3D anatomy and pathology with AR visualization, offering an interactive way for students and healthcare professionals to explore human anatomy and diseases. In addition to apps like VOKA, AR glasses and headsets are becoming crucial tools in surgery. Devices like Microsoft HoloLens and Magic Leap are being used in operating rooms to overlay real-time 3D models onto the surgeon's field of view. As augmented reality in healthcare continues to grow, we can expect even more advancements in both apps and wearable devices.
5. Is AR replacing doctors?
Definitely not. AR is supporting doctors. Augmented reality in healthcare is a tool that enhances visualization, improves accuracy, and helps with training. It can guide surgeries or display vital information in real time, but human expertise, judgment, and empathy remain irreplaceable in patient care.
6. Can AR be used for patient education?
Absolutely. One of the most impactful augmented reality use cases in healthcare is patient education. AR can help explain diagnoses, surgical procedures, and treatment plans through interactive visuals. This improves understanding, reduces anxiety, and supports informed decision-making.
Table of contents
Thank you for your comment!
Your comment has been submitted for moderation and will be published soon. We'll email you once it’s live.